Stacey VanDyke is the director of the nurse anesthesia program at Florida State University’s Panama City Campus. The program trains certified, registered nurse anesthetists (CRNAs), and as VanDyke watched COVID-19 spread earlier this year, the respiratory distress it sparks was a red flag.
Soon, VanDyke realized that CRNA graduates were uniquely positioned to help.
“Among other things, we place breathing tubes, we manage ventilator parameters and settings; we manage airways,” she said. “You see how many (COVID-19) patients need just this kind of care and you realize that CRNAs, graduates of our program, are tailor–made for this environment.”
Before they apply for CRNA training, prospective nurses must work in an intensive care unit so that they’re tested in high-pressure environments. VanDyke said the combination of that experience, plus hands-on training while becoming a CRNA lets the program’s graduates hit the ground running.
With that in mind, she said that CRNA graduates have found themselves working long hours amid long weeks, fighting the virus.
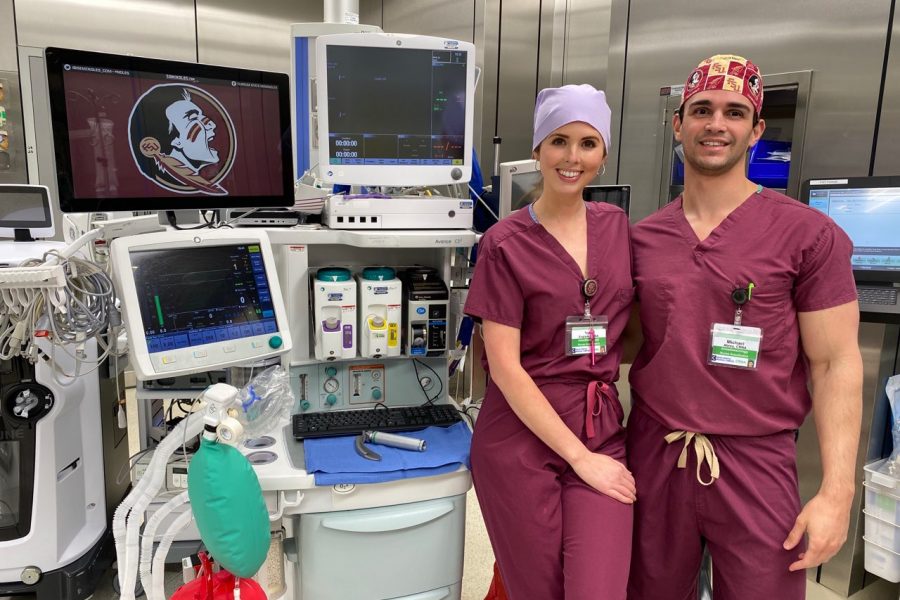
In Falls Church, Virginia 2018 CRNA graduates Michael Abreu and Taylor Englade are engaged to be married. They are also helping to treat COVID-19 patients at Inova Fairfax Hospital.
Abreu said he was like everyone else earlier this year, just watching reports of COVID-19’s spread, before infected patients began arriving at his hospital.
“To finally see it right in front of you, doing the damage it did, that’s an eye-opening moment,” he said. “You realize, this is really real now; I am about to walk into the room with someone who is positive.”
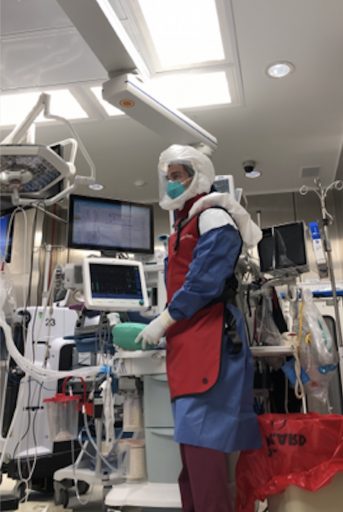
Numerous graduates have felt the call to help and have volunteered, including several who have traveled to New York City, the epicenter of the U.S. outbreak. One of those students, Laura Ketelsen, said she was compelled to put her education and skills to use.
In April, just days after her husband returned from a six–month deployment with the Air Force, Ketelsen left for New York Presbyterian Columbia Hospital, where she’s been treating moderate to severe COVID-19 patients. The volume of patients there forced medical staff to expand their work to an auditorium near the hospital.
“In the ICU, it’s usually one nurse for every two patients,” she said. “But there is no way to manage that ratio with the number of patients right now.”
Before becoming a CRNA, Ketelsen said she worked as an emergency room trauma nurse for five years. While that experience has proved invaluable, the challenges of COVID-19 have surpassed her expectations.
“This feels different because there is so much about this virus that we don’t know,” she said. “We are doing the best we
know how but in other circumstances you know what you’re up against. Because there is so much that we’re still learning, you wonder if there is more you could do, or more you could have done.”
COVID-19 patients present a multitude of symptoms that Ketelsen said makes treating them uniquely challenging.
“This is not just a respiratory infection; the disease affects so many other parts of the body,” she said. “You’ll be in a situation where the ventilator is helping the lungs but then the kidneys fail. One of the big things is blood clotting and a lot of the ICU patients are on blood thinners;

because of that, so many of them end up bleeding. You are trying to address these multiple problems and sometimes the solutions to those problems go against each other.”
She added that despite the challenges she is optimistic: “These patients’ needs are complicated. We are still learning. It’s hard but what we’re learning so far is impressive.”
Ketelsen said she’s working close to 80 hours a week and living out of a nearby hotel. Closed restaurants and millions of residents sheltering in place mean the city is a shadow of its usual, bustling self, but she sees signs of renewal.
The flow of patients is slowing, vehicle traffic is picking up and the team she is working with will soon be able to transition out of the auditorium to a floor inside the hospital.
Englade and Abreu met during their first week of CRNA school and graduated in 2018. While they are now engaged, plans for a wedding will wait.
“Some of the things that seemed so important have vanished,” Englade said. “The superficial things we were looking forward to went to the back of the bus. But we are fortunate enough to go to work.”
Even while working in the same hospital, Abreu and Englade can go entire days without seeing each other. While the hours are long and shared downtime is scarce, each said they try to make time to meet one another for lunch when they can.
VanDyke said Ketelsen, Abreu and Englade are joined by numerous fellow graduates in being on the front line of the fight against COVID-19.
“Many of our alumni have reached out to tell us about their work during this and how they are really able to make a difference,” she said. “They are playing an advanced role, and they are ready for it.”
Ketelsen agreed and added, “This is exactly what I was trained to do.”
For more information about FSU’s CRNA program, visit: https://pc.fsu.edu/nap/program.



